Influenza and Sars-cov-2: strength through unity?
Monitoring SARS-CoV-2 (the etiologic agent of COVID-19) infections is a procedure we are now used to, both as practitioners and as patients. We know our way around molecular, antigenic, and serological tests to detect the presence of a present or past SARS-CoV-2 infection in the body.¹

We also know how the COVID-19 disease has impacted mortality rates. This simple image displaying US epidemiological data from April 2020 shows the impact of the pandemic with respect to the most common causes of mortality. It is evident from this graph that both SARS-CoV-2 infection and “classic” influenza are diseases with a potentially poor prognosis.²

Figure 1. Mortality (new weekly deaths) in the US from COVID-19; data updated to April 2020
The vaccines seem to have provided a good degree of immunity, at least towards the viral variants known at the time of their production, and what we expect for the months ahead is that the virus may do the rounds seasonally like a typical case of flu.³ However, there is still a degree of uncertainty about what will actually happen because of the continued onset and circulation of new viral variants, each with slightly different infectiousness and morbidity characteristics than the previous ones. So far, hundreds of variants of this virus have been identified worldwide, some termed “variants of concern” (VOC) by the WHO, particularly for frail patients:
- The Omicron variant (Variant B.1.1.529) first detected in South Africa on 24 November 2021. Recently found to be predominant in Italy and Europe.
- The Delta variant (Variant VUI-21APR-01, also known as B.1.617) first detected in India.
- The Gamma variant (Variant P.1) originating in Brazil.
- The Beta variant (Variant 501Y.V2, also known as B.1.351) identified in South Africa.
- The Alpha variant (Variant VOC 202012/01, also known as B.1.1.7) first identified in the UK.
Therefore, virological monitoring remains essential both for collecting and updating epidemiological data and for protecting the fragile people we may come into contact with.⁴
Virological surveillance, which has been active for years, maintains for 2022 the already updated “InfluNet” monitoring protocol of the 2020-21 season with some changes from the previous flu season due to the emergency context of the SARS-COV-2 pandemic, with these indications:
- To establish a more widespread surveillance system, with increased enrollment of sentinel doctors (GPs and PCPs) to achieve coverage of at least 4% of the regional population (4% for each local healthcare authority and age group). At the same time, virological surveillance is also called for to be strengthened by increasing the number of swabs taken amongst sentinel doctors’ patients. It would be desirable for all patients of GPs and PLSs with ILIs (Influenza-like illnesses) to be swabbed.
- Since the symptoms of influenza illnesses are comparable to that of Covid-19, it is worthwhile to look for influenza and Sars-CoV-2 viruses on the same swab.
- Regional influenza reference laboratories may also continue to collect a Respiratory Syncytial Virus (RSV) result in clinical specimens tested as part of influenza surveillance.⁵
Even the World Health Organisation in its last congress on the subject held in 2022 highlighted how important it is to proceed with active surveillance, monitoring both SARS-CoV-2 and Influenza and Respiratory Syncytial Virus (RSV).⁶
With the relaxation of restrictions, the problem of co-infections is likely to be prevalent as early as next autumn; in fact, there is evidence that viral co-infections such as those between SARS-CoV-2 and influenza viruses, RSV and adenovirus are often found in seasonal periods.⁷
There is also evidence that prevention is an effective weapon in reducing seasonal exposure to influenza infections: during the SARS-CoV-2 pandemic, the incidence of absolute influenza was reduced overall, and this was as a result of the hygiene standards and restrictions that were adopted. It is believed that advising citizens to get screenings, encouraging their own civic spirit towards the most fragile, is the right way to curb the real healthcare expenditure related to these respiratory diseases.⁸ Current diagnostic investigations should be geared towards detecting both viruses and not just SARS-CoV-2, so that a truly effective respiratory viral infection prevention strategy can be implemented even when RSV is suspected; this is a fairly uncommon respiratory viral disease but one that can especially affect the most fragile individuals.
What happens if you contract a co-infection of SARS-CoV-2 and Influenza?
There are multiple answers to this question because there are several consequences to co-infections. Here are some of them:
- Influenza can make you more susceptible to SARS-CoV-2 due to a reduction in physiological defense capabilities. Influenza worsens your symptoms and the risk of hospitalisation. A very recent study conducted in France and published in the Lancet, shows that patients with SARS-CoV-2/Influenza co-infections are more than four times more likely to require assisted ventilation, and 2.35 times more likely to die than patients with SARS-CoV-2 alone. The research, coordinated in the UK as part of the International Severe Acute Respiratory and Emerging Infection Consortium's (ISARIC) – Coronavirus Clinical Characterisation Consortium, is the largest study ever conducted on people with SARS-CoV-2 and other endemic respiratory viruses, with more than 200,000 patients observed.⁹
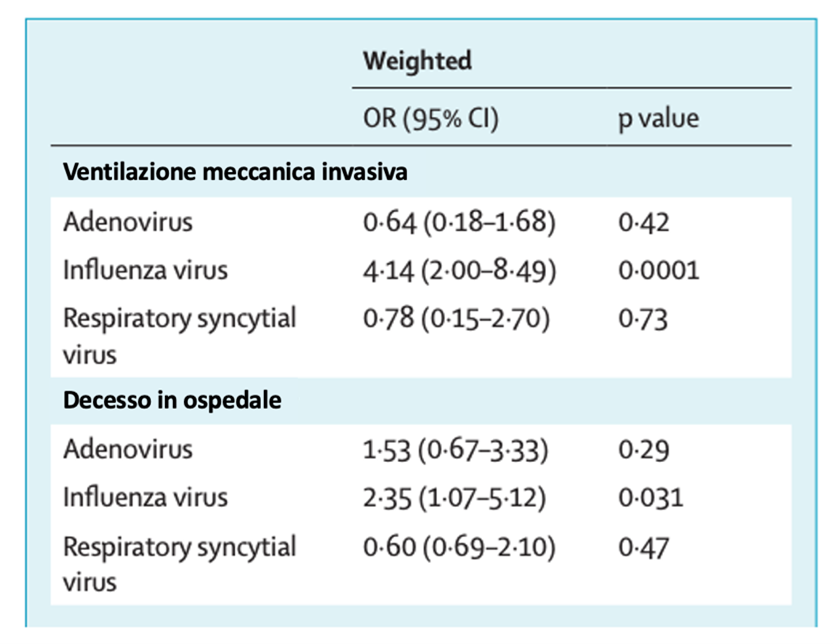
Figure 2. Use of mechanical ventilation and mortality in the UK from February 2020 to
December 2021 in patients with concomitant SARS-CoV-2 co-infection (OR: Odds Ratio)
- Co-infection would appear to be a potential risk factor for the exacerbation of lung damage. In a Chinese study, it is shown that in mice that were pre-infected with influenza A, subsequent infection with SARS-COV-2 causes much greater lung damage by the direct effect on ACE2 receptors.¹⁰
- In general, co-infection of influenza virus and SARS-CoV-2 can cause severe lung infections by other microorganisms for multiple reasons. The influenza virus, for example, increases the infectious potential of opportunistic bacteria, increasing their adherence and invasion ability, making eradicating infections difficult because they require the use of antibiotic therapies and severely debilitate affected patients.¹¹ Modifying the testing strategy for patients with SARS-COV-2 by also expanding the search for influenza much more broadly could therefore be a useful strategy in order to contain other respiratory viral infections and to protect the most fragile population.¹²
The correct and timely identification of Influenza and SARS-COV-2 has practical implications when it comes to managing often similar symptoms and containing the spread of highly transmissible viruses.¹³ The significant increase in risk for patients with co-infection has several implications and suggests that patients hospitalised for SARS-CoV-2 disease should be subjected to dual testing to identify them as potentially more fragile , interpret immunomodulatory responses, or send them for personalised antiviral therapy.
Nasopharyngeal/oropharyngeal swabbing for symptomatic patients can be used to simultaneously detect SARS-CoV-2 Virus, Influenza A and B Viruses, and Respiratory Syncytial Virus-specific genes via the Real Time PCR method. Co-testing for SARS-CoV-2 and other respiratory pathogens such as those indicated using swabs performed on symptomatic patients, is also strongly recommended in the recently published InfluNet 22-23¹⁴ protocol within the context of the Epidemiological and Virology Surveillance by the Supreme Health Council (ISS). As of today, there are highly sensitive molecular tests on the market that can provide a definitive qualitative answer in a short period of time and ensure maximum efficiency of laboratory workflow, such as the BD SARS-Cov-2/Flu test (with the possibility of also detecting RSV in the same reaction) for the BD MAX™diagnostic system.
DOWNLOAD THE BD MAX™ RTI SOLUTIONS BROCHURE™
BD-73771
Bibliography
1. Ong DSY, Fragkou PC, Schweitzer VA, Chemaly RF, Moschopoulos CD, Skevaki C; European Society of Clinical Microbiology and Infectious Diseases (ESCMID) Study Group for Respiratory Viruses (ESGREV). How to interpret and use COVID-19 serology and immunology tests. Clin Microbiol Infect. 2021 Jul;27(7):981-986.
2. Schulman A. et al, Not Like the Flu, Not Like Car Crashes, Not Like – The New Atlantis. 2020
3. Chotpitayasunondh T, Fischer TK, Heraud JM, Hurt AC, Monto AS, Osterhaus A, Shu Y, Tam JS. Influenza and COVID-19: What does co-existence mean? Influenza Other Respir Viruses. 2021 May;15(3):407-412.
4. Prevalenza e distribuzione delle varianti di SARS-CoV-2 di interesse per la sanità pubblica in Italia. Epicentro ISS. Rapporto 10 dicembre 2021
5. InfluNet & CovidNet. Sistema di Sorveglianza Sentinella delle sindromi simil- influenzali, dei virus influenzali e del virus Sars-CoV-2
6. McKimm-Breschkin JL, Hay AJ, Cao B, Cox RJ, Dunning J, Moen AC, Olson D, Pizzorno A, Hayden FG. COVID-19, Influenza and RSV: Surveillance-informed prevention and treatment – Meeting report from an isirv-WHO virtual conference. Antiviral Res. 2022 Jan;197:105227.
7. Swets MC, Russell CD, Harrison EM, Docherty AB, Lone N, Girvan M, Hardwick HE; ISARIC4C Investigators, Visser LG, Openshaw PJM, Groeneveld GH, Semple MG, Baillie JK. SARS-CoV-2 co-infection with influenza viruses, respiratory syncytial virus, or adenoviruses. Lancet. 2022 Apr 16;399(10334):1463-1464.
8. Stamm P, Sagoschen I, Weise K, Plachter B, Münzel T, Gori T, Vosseler M. Influenza and RSV incidence during COVID-19 pandemic-an observational study from in-hospital point-of-care testing. Med Microbiol Immunol. 2021 Dec;210(5-6):277-282.
9. Swets MC, Russell CD, Harrison EM, Docherty AB, Lone N, Girvan M, Hardwick HE; ISARIC4C Investigators, Visser LG, Openshaw PJM, Groeneveld GH, Semple MG, Baillie JK. SARS-CoV-2 co-infection with influenza viruses, respiratory syncytial virus, or adenoviruses. Lancet. 2022 Apr 16;399(10334):1463-1464.
10. Bai L, Zhao Y, Dong J, Liang S, Guo M, Liu X, Wang X, Huang Z, Sun X, Zhang Z, Dong L, Liu Q, Zheng Y, Niu D, Xiang M, Song K, Ye J, Zheng W, Tang Z, Tang M, Zhou Y, Shen C, Dai M, Zhou L, Chen Y, Yan H, Lan K, Xu K. Coinfection with influenza A virus enhances SARS-CoV-2 infectivity. Cell Res. 2021 Apr;31(4):395-403.
11. Musher DM. Bacterial Coinfection in COVID-19 and Influenza Pneumonia. Am J Respir Crit Care Med. 2021;204(5):498-500. doi:10.1164/rccm.202106-1467ED
12. Saul H, Gursul D, Antonelli M, Steves C. Frail older people and those in deprived areas remain at risk from covid-19, even after vaccination. BMJ. 2022 Jul 4;378:o1313.
13. Pormohammad A, Ghorbani S, Khatami A, Razizadeh MH, Alborzi E, Zarei M, Idrovo JP, Turner RJ. Comparison of influenza type A and B with COVID-19: A global systematic review and meta-analysis on clinical, laboratory and radiographic findings. Rev Med Virol. 2021 May;31(3):e2179.
14. Operational protocol – InfluNet & RespiVirNet season 2022-23 – https://w3.iss.it/site/RMI/influnet/pagine/Documenti.aspx (Viewed on 17 October 2022)
